Social Communication Disorder is a persistent difficulty with the social use of verbal and nonverbal communication, such as taking turns in conversation, reading context, or understanding sarcasm, and it does not include the restricted or repetitive behaviors required for an autism diagnosis. It was introduced in the DSM-5 in 2013, and as a standalone diagnosis it appears to be rare, with population studies finding less than 1% prevalence when autism-related symptoms and structural language issues are excluded.
If you're searching what is social communication disorder, you may already know the feeling that something goes wrong in conversation even when your intentions are good. You reply overly precisely. You miss that someone wants to change the subject. You explain too much to one person and not enough to another. Then you replay the exchange for hours, wondering what everyone else seemed to catch so easily.
That experience can feel lonely, but it isn't laziness, rudeness, or a lack of caring. Social communication has hidden rules, and some people have real difficulty noticing, interpreting, and using those rules in real time. For adults, teens, parents, and educators, understanding those hidden rules is often the first relief.
The Invisible Hurdles of Conversation
A lot of people think communication problems are always obvious. They imagine someone who can't speak clearly or doesn't have the words. But many social communication struggles are much quieter than that.
You might have a strong vocabulary and still leave conversations confused. A child might speak in full sentences and still struggle to join a game. A teenager might desperately want friends and still keep missing the tone of a joke, the pause that signals "your turn," or the facial expression that means "please stop."
That is part of what is social communication disorder. It often shows up not in the words themselves, but in the social meaning around the words.
> Practical rule: If someone can talk, read, or write fairly well but keeps stumbling over the unwritten rules of interaction, it makes sense to look at social communication, not just language skill.
These hurdles are "invisible" because other people often misread them. They may call the person blunt, immature, odd, self-focused, dramatic, careless, or shy. The person with the difficulty may start believing those labels too.
Sometimes the clearest way to understand this is to stop asking, "Why is this person making conversation hard?" and start asking, "What part of the social code are they being expected to decode on the fly?" If that question feels familiar, this reflection on why communication can feel so hard in everyday life can help put words to the strain.
Why it hurts so much
Conversation isn't just about exchanging information. It's how people build safety, belonging, and trust. When that process keeps going off track, the result isn't only awkwardness. It can become anxiety, self-doubt, conflict, and withdrawal.
Many people with these difficulties grow up hearing some version of:
- "You know better." Even when they didn't catch the social cue.
- "That was rude." Even when they were trying to be honest.
- "You're too much." Even when they were unsure how much detail the moment called for.
Those repeated moments can shape identity. People stop trusting their instincts. They enter conversations bracing for mistakes.
Unpacking Social Communication Disorder
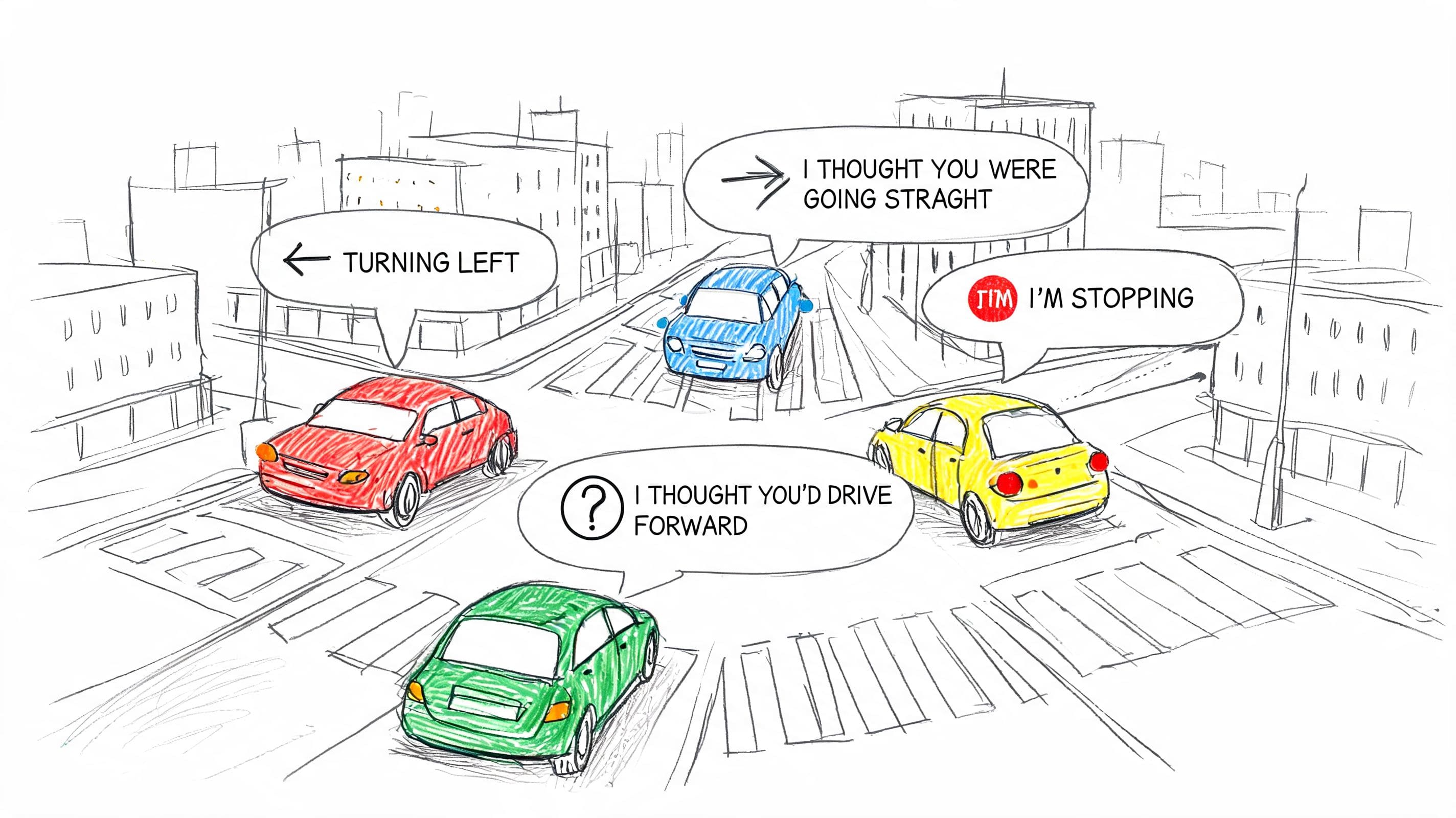
A useful way to understand Social Communication Disorder, or SCD, is to think about driving. Some people know how to operate the car just fine. They can steer, brake, and follow the map. But they struggle with the unwritten traffic rules. Who goes first at a messy intersection? When is a pause an invitation? When does "fine" mean "I'm upset"?
That's what pragmatics often feels like. Not the mechanics of language, but the social rules of using it.
According to a plain-language overview of Social Communication Disorder and DSM-5 criteria, the condition includes four core areas: difficulty using communication appropriately in social contexts, difficulty following conversation rules like turn-taking, difficulty understanding non-literal language such as sarcasm or idioms, and difficulties serious enough to affect relationships, participation, or daily functioning.
What the diagnosis means in plain English
Here is the simplest translation of those criteria into everyday life.
- Using communication for social purposes is hard.
A person may know many words but struggle with why and how to use them in a moment. They might give a lecture when the other person wanted comfort, or answer a casual question with a level of detail that doesn't fit the setting.
- Adjusting communication to the situation is hard.
The same style may show up everywhere. A student may talk to a principal exactly as they talk to a sibling. An adult may write work emails that sound too abrupt, too formal, or too personal because the "right register" doesn't come naturally.
- Following conversation rules is hard.
This can look like interrupting, changing topics suddenly, missing when someone is bored, failing to repair a misunderstanding, or not knowing how to enter or leave a group conversation smoothly.
- Understanding implied meaning is hard.
Idioms, teasing, vague hints, indirect requests, and sarcasm can all become traps. "Can you get that?" may sound like a question about ability rather than a request. "Wow, nice one" may be understood at face value even when the tone means the opposite.
The four skill areas underneath it
Many clinicians and educators think about SCD through four broad lenses:
| Area | What it affects in real life |
|---|---|
| Pragmatics | Knowing what to say, how much to say, and when to say it |
| Social interaction | Managing back-and-forth exchange with one person or a group |
| Social cognition | Inferring what other people might mean, feel, expect, or assume |
| Language processing | Pulling together words, tone, gesture, and context into one message |
A child can look verbally bright and still struggle in all four. An adult can sound articulate in meetings and still leave not knowing whether a coworker was annoyed, joking, or hinting at a problem.
> Good communication isn't just "saying words correctly." It's matching words, tone, timing, and context.
What SCD is not
SCD isn't the same as being shy. Shy people often understand the social rules but feel anxious about using them. SCD isn't bad manners either. Manners involve choice. Social communication difficulties often involve missing the cue in the first place.
It also isn't a sign that someone doesn't care about others. In many cases, the opposite is true. The person may care a great deal and still struggle to read the moment accurately.
If you're supporting a child and want broader emotional development context alongside communication support, these key insights for parents and teachers offer a helpful companion perspective.
Recognizing the Signs Across the Lifespan
Social communication difficulties don't look exactly the same at every age. The core challenge may stay similar, but life asks different things of a child on a playground, a teenager in a group chat, and an adult in a workplace.

Research also points to a wider impact than many people realize. A review on overlooked emotional and developmental aspects of SCD notes that beyond communication itself, people may also experience impaired emotion regulation, a weaker sense of agency, and challenges with self-development. That matters because many families focus on "social skills" while missing the emotional wear and tear underneath.
In childhood
In younger children, SCD may hide behind a sentence like, "But they talk all the time." Adults often assume frequent talking means communication is developing smoothly. Sometimes it is. Sometimes it isn't.
A child may speak clearly and still have trouble with the social side of play. They may talk at peers instead of with them. They may miss the rhythm of pretend games, not notice when another child wants a turn, or answer questions in ways that stop the interaction instead of keeping it going.
Common childhood patterns can include:
- Literal responses when classmates are joking or pretending.
- One-sided talking that sounds more like broadcasting than sharing.
- Trouble joining games because the rules of entry are unwritten.
- Missing facial expressions or tone that other children use to negotiate play.
Adults sometimes call this bossy, awkward, or immature. A more useful question is whether the child understands the hidden structure of the interaction.
In adolescence
Adolescence raises the difficulty level. Social life becomes faster, less direct, and much more dependent on nuance. Friends use inside jokes, irony, shifting alliances, and vague language. Teenagers are often expected to "just know" what a text means, what a glance means, or when silence means discomfort.
A teen with SCD may do well in academic tasks and still feel lost socially. They may miss flirting, misunderstand teasing, sound too intense in group chats, or reveal too much personal information because they can't easily gauge what level of closeness is appropriate.
That can create a painful loop:
1. A teen misreads a social moment.
2. Peers react negatively or drift away.
3. The teen becomes more anxious and self-conscious.
4. Future conversations become even harder.
Some teens also start masking. They memorize phrases, copy peers, or stay quiet to avoid mistakes. That effort can be exhausting. If you're trying to make sense of what happened in a confusing exchange, this guide to how to interpret a social situation more clearly can help break interactions into smaller, more understandable pieces.
> Many teens aren't "not trying." They're trying so hard that they go home depleted.
In adulthood
Adult signs are often missed because the person has had years to compensate. They may have scripts for introductions, a polished professional voice, or a habit of staying out of group conversations. Other people may only notice the moments when repair breaks down.
At work, this can look like misreading indirect feedback, giving too much detail in meetings, sounding blunt in email, struggling with small talk, or not realizing a coworker is trying to end the conversation. In friendships or dating, it may show up as difficulty reading mixed signals, trouble balancing reciprocity, or confusion about what level of honesty is expected in a given moment.
Adults often describe the experience in emotional terms before they ever use diagnostic language:
- "People keep misunderstanding my tone."
- "I only realize later that I said too much."
- "I can do the job. The people part is what drains me."
- "I don't know why everyone else seems to read the room faster."
Those are not small complaints. They affect belonging, confidence, and opportunities.
SCD vs Autism and Other Conditions
Confusion about diagnosis is common because several conditions can affect communication. The overlap is real. The distinctions still matter.
A careful comparison helps.
SCD vs ASD vs Language Disorder at a glance
| Feature | Social Communication Disorder (SCD) | Autism Spectrum Disorder (ASD) | Language Disorder |
|---|---|---|---|
| Main difficulty | Social use of language and nonverbal communication | Social communication differences plus restricted or repetitive behaviors | Language form or content, such as vocabulary, grammar, or sentence structure |
| Conversation style | May struggle with turn-taking, context, implied meaning, or audience awareness | May have similar social communication challenges | May struggle to express ideas clearly because of language mechanics |
| Sarcasm and idioms | Often difficult | Can also be difficult | May be difficult if language comprehension is broadly affected |
| Restricted interests or repetitive behaviors | Absent as a required feature | Present as part of diagnosis | Not a defining feature |
| Why assessment matters | Needs to be separated from autism and other language concerns | Broader developmental picture is considered | Focus is on language structure and understanding |
The key difference from autism
The most important distinction is this: SCD does not include the restricted or repetitive behaviors required for autism spectrum disorder.
Someone with SCD may struggle at a noisy party because the social chatter is hard to track. Someone with autism may have that same difficulty and also show restricted interests or repetitive behaviors that are part of the diagnostic picture. That difference is why clinicians don't diagnose SCD when autism better explains the pattern.
A review of prevalence and differential diagnosis for Social Pragmatic Communication Disorder found that isolated SCD is rare, with population studies showing less than 1% prevalence when structural language difficulties and autistic symptoms are excluded. In clinical settings, among children referred for autism evaluation, about 8% met criteria for SCD. That makes precise differential diagnosis essential.
How SCD differs from a language disorder
A language disorder usually affects the structure or content of language itself. A person may struggle with grammar, vocabulary, sentence formulation, or understanding spoken language. SCD is different. The person may have the words, but not the social map for using them.
Think of it this way. A language disorder often affects building the sentence. SCD often affects using the sentence in the right way for the right person at the right moment.
Where ADHD complicates the picture
ADHD can muddy the waters because attention, inhibition, and working memory all affect conversation. Someone may interrupt because of impulsivity, miss cues because they were distracted, or lose the thread because of executive function overload. That doesn't automatically mean SCD. It means the pattern needs careful interpretation.
Some readers come to this question through early language worries. If that's your path, practical milestones like encouraging your baby's first words can be useful for understanding typical communication development before social-pragmatic differences become clearer.
For readers comparing broader neurodevelopmental profiles, this guide to autism and communication differences can help clarify where overlap ends and where the conditions differ.
The Path to Clarity Assessment and Diagnosis
A diagnosis often starts with a familiar scene. Someone can speak clearly, has plenty to say, and may even do well one on one. Then a group discussion, classroom exchange, family gathering, or work meeting goes sideways. They miss the hidden rules of the moment, and everyone leaves with a different interpretation of what just happened.

That gap is often what assessment is trying to explain. The goal is more than attaching a label. The goal is to identify where communication breaks down, what skills are strong, what situations create the most strain, and which supports would make daily life easier.
Who evaluates SCD
A speech-language pathologist often takes the lead because SCD involves the social use of language, not just speech sounds or vocabulary. Psychologists, developmental specialists, pediatricians, psychiatrists, and school teams may also be part of the process, depending on the person's age and the setting.
This team view matters because social communication can be affected by several overlapping issues. A careful evaluator is sorting through patterns over time, across settings, and across demands. That is why one brief appointment rarely gives the full picture.
What a thorough assessment includes
A strong evaluation usually pulls together several kinds of evidence, a bit like putting together a map instead of judging the whole trip from one wrong turn.
- Developmental history
Clinicians ask about early communication, play, friendships, school experiences, work challenges, and the situations that create repeated misunderstandings.
- Observation across contexts
Someone may sound confident in a quiet office but struggle to read timing, subtext, or turn-taking in faster, less predictable settings.
- Structured tasks and pragmatic measures
These can show whether the person has trouble with inference, repairing a misunderstanding, shifting language for different listeners, or reading nonverbal signals.
- Reports from people who know the person well
Parents, teachers, partners, supervisors, and the individual themselves often notice patterns that never appear during a short clinic visit.
Good assessment also looks at impact. Does the person avoid group work because it feels chaotic? Do friendships stall after repeated misread cues? Does workplace feedback sound vague, such as "great skills, but communication is off"? Those real-life examples matter because diagnosis should connect to daily function, not stay trapped in clinical language.
Why the process can feel confusing
Many teens and adults reach assessment after years of hearing mixed messages. They may be described as bright, verbal, thoughtful, blunt, immature, intense, shy, or awkward, sometimes all at once. That can make the experience feel personal rather than medical.
There is also a practical problem. Social rules are often taught as if everyone absorbs them automatically. For people with SCD, those rules can feel like a conversation happening one step too fast. By the time they realize a cue was missed, the moment is gone.
That is why a good evaluation should leave you with more than a yes or no answer. It should explain what is happening in plain language and point toward support you can use. If stress, burnout, or anxiety are part of the picture, broader guidance on understanding your mental health needs can help you decide whether communication assessment should happen alongside mental health support.
If appointments leave you feeling dismissed, this guide on how to advocate for yourself in health and support settings can help you prepare examples, ask better questions, and request a fuller evaluation.
Actionable Strategies for Clearer Communication
Once people understand what is social communication disorder, the next question is usually more urgent: what actually helps?
The short answer is structure. Social communication skills often don't grow best through vague advice like "just watch what other people do." They improve when the hidden rules are made visible, practiced directly, and used in real situations with support.
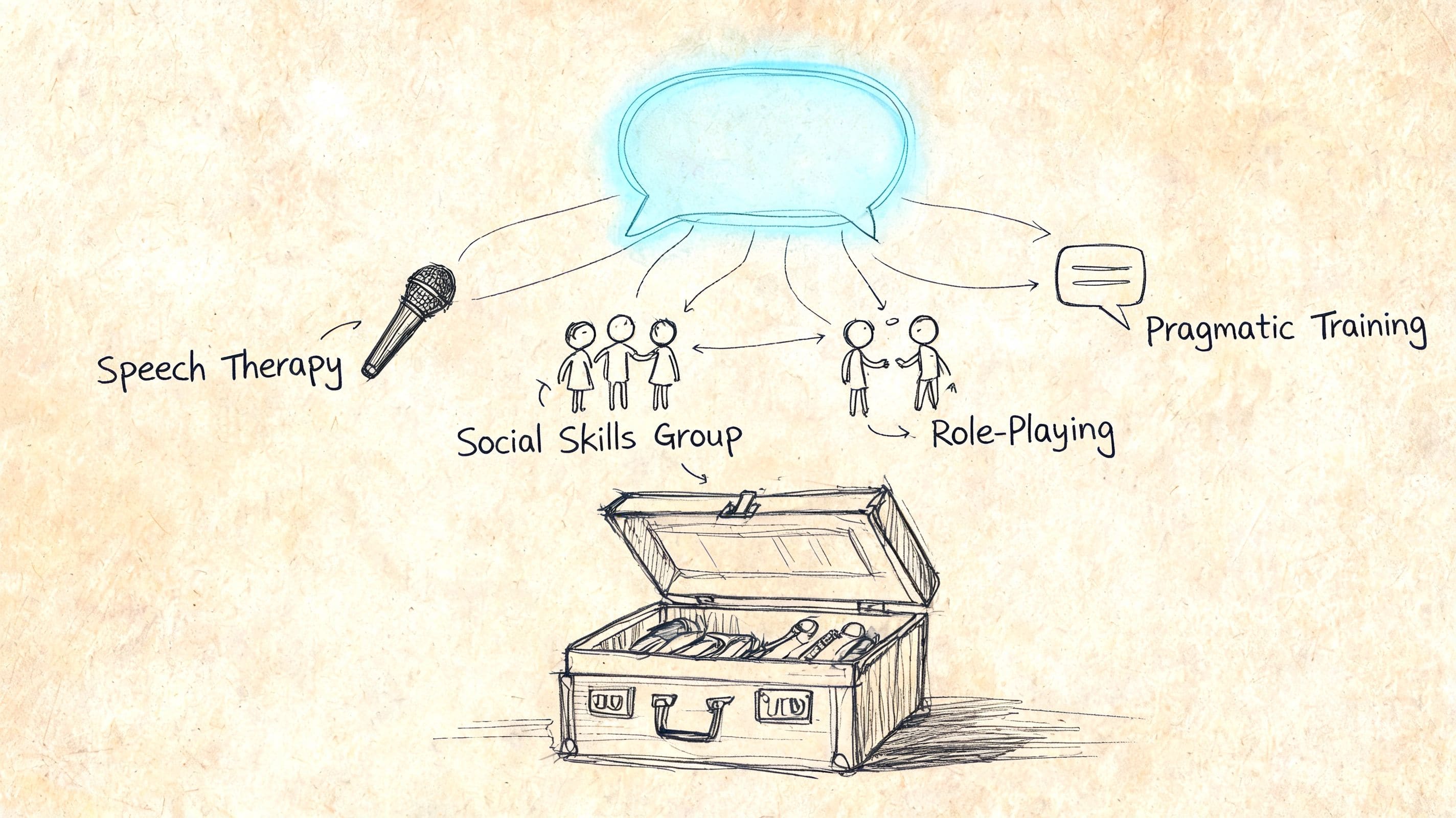
Therapy that targets the real problem
Speech-language therapy is often the most direct support because it can focus on pragmatics, not just speech sounds or vocabulary. That may include practicing conversational openings, topic shifts, repair strategies, understanding implied meaning, or noticing how tone and body language change meaning.
Other supports can matter too:
- Social communication groups help people practice with peers in a more realistic setting.
- Cognitive behavioral therapy can help with the anxiety that often builds around repeated misunderstandings.
- Parent and caregiver coaching can make practice more consistent and less stressful at home.
- Classroom and workplace supports can reduce hidden expectations and make communication more explicit.
What support looks like day to day
Good support isn't only "therapy time." It also changes how daily communication is handled.
A few examples:
1. Use direct language when possible
Instead of hinting, say the need clearly. "Please send me the draft by Friday" is easier to process than "It would be great to have this soon."
2. Teach scripts, then adapt them
Scripts can help with greetings, asking for clarification, joining a group, ending a conversation, or repairing a misunderstanding. They aren't cheating. They're scaffolding.
3. Break social tasks into parts
"Have better conversations" is too vague. "Ask one follow-up question, pause, then check the other person's expression" is teachable.
4. Review real interactions afterward
Calm reflection helps the person connect the dots: what was said, what was implied, what cues were missed, and what could be tried next time.
> Structure lowers cognitive load. When the brain isn't scrambling to decode everything at once, learning becomes possible.
Helpful accommodations at school, home, and work
Support gets stronger when environments change too.
- At school
Teachers can give explicit instructions for group work, explain figurative language, and avoid assuming that a student "should know" the social expectation.
- At home
Caregivers can model how context changes communication. The same message can be compared across situations: friend, teacher, grandparent, coach.
- At work
Managers can give direct feedback, clarify unwritten norms, and make room for written follow-up after meetings.
That approach is often more effective than trying to force a person to absorb social rules by osmosis. Clear expectations help. Concrete examples help. Rehearsal helps.
Progress can look different than people expect
Improvement doesn't always mean becoming effortlessly social. Sometimes it means noticing confusion sooner. Sometimes it means asking, "Do you mean that exactly?" Sometimes it means learning how to pause before oversharing, or how to say, "I'm not sure what tone you meant."
Those are meaningful gains because they reduce friction and increase self-trust.
Essential Resources for Support and Learning
The right resource can lower a lot of confusion. A parent may be trying to understand why group projects keep going sideways. A teen may know conversations feel hard but not have words for why. An adult may be exhausted from guessing what other people meant all day.
Different people need different kinds of help.
For parents and caregivers
Start with sources that explain social communication in plain language and connect it to daily life, not just diagnostic terms. Professional guidance from speech-language organizations can help you understand what clinicians look at, how pragmatic language works, and which questions to bring to an evaluation.
It also helps to build a small support team around the child. A pediatrician, school staff member, or speech-language pathologist can help sort out what is happening first, especially when social misunderstandings are tangled up with anxiety, frustration, or school stress.
For neurodivergent adults
Adults often need resources that speak to real-world pressure points: dating, friendship, interviews, office politics, texting, and group conversations that shift too fast. Child-focused descriptions can miss that experience.
Useful support may include a speech-language pathologist who works with teens and adults, a therapist who understands social fatigue, or practical tools that reduce the load of decoding tone and intent in the moment. This guide to apps for neurodivergent communication support is a helpful place to compare options for everyday conversation stress.
Sometimes the best resource is not more information. It is a tool, script, or accommodation that makes one hard part easier today.
For clinicians and educators
Clinicians and educators often need a shared framework. Social communication works a bit like traffic flow. The words themselves are only part of it. Timing, turn-taking, context, and unwritten rules shape whether the message gets through clearly.
That is why examples from real settings matter so much. Teacher observations, family descriptions, and notes about what happens in class, at lunch, online, or during unstructured conversation can reveal patterns that a formal task may miss. Shared language across home and school also makes support more consistent, which helps the person learning these skills feel less lost and less blamed.
Frequently Asked Questions about Social Communication Disorder
Can you be diagnosed with SCD as an adult
Yes, adults can still be identified, even though many descriptions focus on children. The challenge is that adult diagnosis is often less straightforward. People may have spent years masking, memorizing scripts, or avoiding situations that expose the difficulty.
Adult assessment also requires care because symptom overlap can blur the picture. A discussion of SCD, adult diagnosis, and overlap with ADHD notes that pragmatic issues in SCD can resemble features seen in autism or can be influenced by ADHD-related executive function difficulties. That doesn't make adult diagnosis impossible. It means clinicians need a detailed history and careful differential diagnosis.
What's the overlap between SCD and ADHD
There can be real overlap in daily experience. A person with ADHD may interrupt, lose track of a conversation, miss social cues, or respond too fast. A person with SCD may also interrupt or miss cues, but for a different reason. The core issue may be social inference and pragmatic understanding rather than attention or inhibition alone.
In real life, the two can coexist. That's one reason people often feel confused by labels. The same outward behavior can come from different underlying difficulties.
Why can't someone just learn social skills by watching others
Because observation alone often isn't enough when the difficulty lies in interpreting social meaning. If a person can't reliably infer why one phrase worked in one context and failed in another, "just watch and copy" becomes frustrating.
This is one of the most misunderstood parts of SCD. People may assume that repeated exposure should automatically teach the pattern. For many individuals, it doesn't. Structured, explicit teaching works better because it names the rule, gives examples, and allows practice with feedback.
> Watching social interaction isn't the same as decoding it.
Does SCD affect only spoken conversation
No. Social communication reaches across spoken, written, and nonverbal interaction. The same person who struggles with sarcasm in conversation may also misread email tone, send messages that sound harsher than intended, or miss what a gesture or facial expression is communicating.
That broad impact is why support should be practical, not abstract. The goal isn't to make someone perform a fake version of "normal." It's to help them understand context, express themselves more clearly, and feel less lost in interactions that matter.
If social situations leave you second-guessing your tone, replaying conversations, or wishing you had the right words sooner, tonen can help you communicate with less stress. It offers a Scripts Library with 188+ ready-to-use prompts, a Perspective Helper for thinking through what someone might mean, Practice Mode for low-pressure rehearsal, and a Calm Kit for moments of overwhelm. It was built by neurodivergent makers, keeps your conversations on your device, and is designed to lower the mental load of everyday communication.